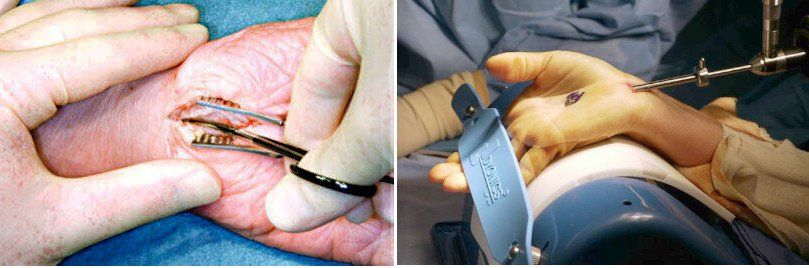
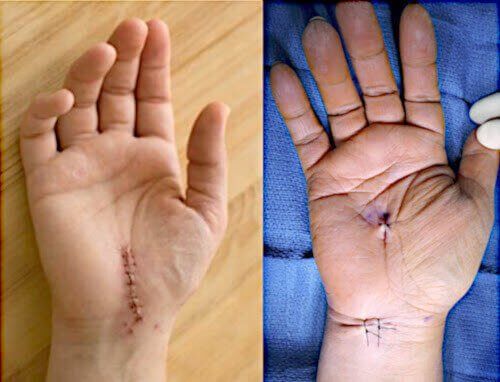
6 Bad Results of Carpal Tunnel Surgery
From Dr. Z - Carpal tunnel syndrome specialist
Overall Results of Carpal Tunnel Surgery
Your results of carpal tunnel surgery can vary from complete failure to complete success. Usually it's somewhere in the middle. The ultimate outcome depends on several factors, some of which are not in your control.
But most people are usually concerned about surgical failure. Below are the 6 most likely reasons your carpal tunnel surgery can fail.
In the end, the best definition of success or failure is how satisfied you are with the outcome. In most cases, this will not be an immediate conclusion. That's because most patients need several months (or even years) after surgery to conclude if their final results turned out good or bad.
- FIND OUT: do you have carpal tunnel? No strings attached self-test.
What determines successful results of carpal tunnel surgery?
Do you know what "surgical success” means? It actually depends on who you ask: a doctor or a patient.
- If you ask a hand surgeon what success means, they’ll say the surgery was successful if they cut the transverse carpal ligament in half without complications. On rare occasion the ligament is not completely cut in half. And that means carpal tunnel symptoms remain. Other times, there are complications like excessive bleeding. These constitute surgical failures. Since these problems happen only 2-4% of the time surgeons say the operation has a 96-98% overall success rate.
- If you ask a patient what success means you’ll get a completely different definition. Usually, it relates to the patient’s satisfaction with their final results. In that regard, when surveyed, only about 50% of carpal tunnel patients are satisfied with their surgical outcome by year 2-3. That translates into a 50% overall success rate of the surgery.
Those are big differences in definitions! Perhaps the fairest (and most easily measured) definition of surgical “failure” is the patient’s ultimate overall assessment. After all, it's the patient's opinion that matters most.
Most pain doctors have a completely different definition. They say a "surgical failure” is when the patient’s carpal tunnel symptoms don’t resolve well enough by 3 months after surgery. These are called persistent symptoms. (Other medical surveys use a 12 or 24 month benchmark - but results are identical.)
Ways carpal tunnel surgery can fail
The results of carpal tunnel surgery are considered a failure by the third year when:
- Symptoms simply didn’t resolve for some unknown reason.
- One or more symptoms returned immediately after surgery.
- Symptoms progressively worsened over time.
- Post-surgical pain is intense and prolonged.
Doctors say the 6 most likely REASONS your carpal tunnel release surgery can fail are as follows:
- Incomplete cut of the transverse ligament due to surgeon error.
- Nerve damage due to surgeon error.
- Blood vessel damage due to surgeon error.
- Unanticipated involvement of another disorder (like diabetes, rheumatoid arthritis)
- Patient non-compliance (like returning to a job that over-stresses the hand).
- Prolonged pain or excessive scarring.
*Sources
- J.C.E. Lane, et. al. (2020) Serious postoperative complications and reoperation after carpal tunnel decompression surgery....
- Johns Hopkins Medicine (2020) Carpal tunnel release
- M. Van, et. al. (2019) Failed carpal tunnel surgery: A guide to management
The consequences of surgical failure
When the surgery fails there are few options remaining. Less than 40% of patientsreturn for another carpal tunnel surgery, called "revision surgery".
By any measure used, the failure rate of a revision surgery is usually much higher than the first surgery. The current estimate is that about 80%of those revision surgeries fail.
Generally, when the results of carpal tunnel surgery lead to failure, the patient is back to square one again. But in many ways, the problem is worse.
- There’s an added financial burden from the first surgery.
- The patient lost job time and (probably) wages.
- Pain and suffering continues.
- The experience takes an emotional toll on the patient.
Therefore, considering a second carpal tunnel surgery after the first one failed creates a real dilemma. This is why most patients decide to not undergo a second operation.
When results see symptoms return
Approximately 30% of patients who have carpal tunnel release surgery see their symptoms initially resolve. However, symptoms return within 2 years.
Again, surgeons don’t consider this a “failed surgery”. That's because patients had a 2 year respite from the pain and numbness after the procedure.
Return of symptoms is emotionally draining because patients believed the problem would be a thing of the past after surgery. Now they have to re-visit the problem once again. While relatively few patients consider having surgery a second time, the decision to do so is both traumatic and financially burdensome.
When symptoms happen on the other hand
Insurance reimbursement nightmares
Having the actual hand surgery and subsequent rehabilitation is one thing; getting it paid for is another. The American Journal of Occupational Health found 79% of carpal tunnel surgery claims were initially rejected by workers’ compensation underwriters.
Also, the average time from filing a claim to obtaining workers’ compensation approval for surgery was 11 months. So don't expect immediate compensation.
This delay, and the associated paperwork, adds even more stress to the financial and emotional stability of the patient and their family. So what happens if the surgery fails? Generally, every difficult challenge the patient had to endure must be repeated. And if symptoms also start on the other hand , the patient must consider surgery on the other hand even more carefully.
Finally, getting Medicare to pay for the surgery is either easy or difficult, depending on your state. Medicare pays only for carpal tunnel surgery that's "medically necessary". And there certainly will be out-of-pocket expenses you will incur.